Health News
Latest quarterly healthcare report provides new insights on longer stays for overnight admitted patients in NSW public hospitals

Health News
Vape Laws Spark Opposition

Health News
Onsite Pharmacists – Just What the Doctor Ordered

Health News
Foods That Can Help Reduce or Prevent Joint Pain

-

 Tweed Shire News2 years ago
Tweed Shire News2 years agoA NEW TWEED HEADS
-

 Motoring News1 year ago
Motoring News1 year agoToyota Supra: Get Ready For A Fully Electric Version In 2025
-
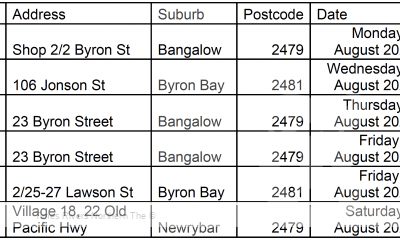
 COVID-19 Northern Rivers News3 years ago
COVID-19 Northern Rivers News3 years agoNorthern Rivers Local Health District COVID-19 update
-

 COVID-19 Northern Rivers News3 years ago
COVID-19 Northern Rivers News3 years agoNorthern Rivers COVID-19 update
-

 Northern Rivers Local News3 years ago
Northern Rivers Local News3 years agoFears proposed residential tower will ‘obliterate’ Tweed neighbourhood’s amenity and charm
-
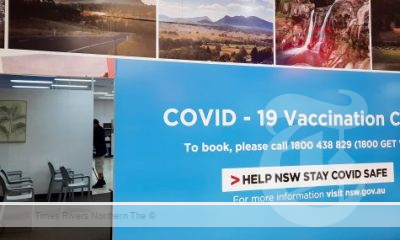
 Health News3 years ago
Health News3 years agoCOVID-19 Vaccination Clinic now open at Lismore Square
-

 COVID-19 Northern Rivers News3 years ago
COVID-19 Northern Rivers News3 years agoLismore Family Medical Practice employee close contact
-

 NSW Breaking News3 years ago
NSW Breaking News3 years agoVale: Former NSW prison boss Ron Woodham

























